The following is taken with kind permission from the Pitt Hopkins Research Foundation website.
Author: Raoul Hennekam MD PhD, Professor of Paediatrics and Translational Genetics, University of Amsterdam, The Netherlands, Summer 2010
Appearance
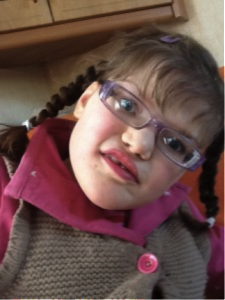
- Head: people with PTHS have a small head circumference, and their forehead recedes compared with the cheeks and jaw.
- Nose: the base of the nose is broad, the tip of the nose full, and the nostrils (alae) of the nose often flare.
- Mouth: the mouth is broad with a large cupid’s bow, the lips often look pouted; full lower lip.
- Ears: prominent ears with thick outer edges (helices).
- Fingers and toes: fingers are often wide and rounded with raised finger nails (clubbed fingers); fetal pads of fingers and toes (where your finger prints are) can be more fleshy than normal.
- Growth: most children grow slowly and at their full heights are slightly shorter than their family members.
Medical symptoms
- Low muscle tone (hypotonia).
- Hypotonia can cause feeding problems and slow motor development in infants and children.
- A combination of low muscle tone and a lack of physical co-ordination (ataxia) means that children often learn to walk at a later age than children without PTHS and have a wide, stiff gait.
- Physical therapy and speech therapy from an early age can be very useful.
- Unusual breathing patterns: this is typically a few minutes of very fast breathing (hyperventilation), followed by a few minutes where the child breathes very slowly or their breath pauses (apnoea). This pattern is sometimes repeated in a short space of time. Alternatively, hyperventilation (hyperbreathing) or apnoea can appear by themselves. Doctors think that these episodes might be caused by excitement or anxiety because they only happen when the child is awake. During hyper breathing, the child can swallow a lot of air, which causes a distended stomach. This symptom normally appears between the ages of 5 and 10 years. In some cases this symptom does not start until adulthood.
- Constipation: in most cases this is chronic. One child’s constipation was caused by the abnormal function of the nerves in the gut wall (Hirschsprung disease). The cause of constipation in most children is unknown.
- Epilepsy. This is a less common symptom of PTHS. It is usually successfully treated by anti-epileptic medication. Epilepsy can usually be diagnosed with an EEG or a brain MRI. In people with PTHS, epilepsy is caused by under development of the structure that links the two halves of the brain (corpus callosum) and a convex nucleus caudatus.
Behavioural symptoms
- Children with PTHS are always moving and busy. Many children flap their hands when they are excited. They are normally devoted, happy and cheerful children and can have bouts of laughter with no clear reason for this. Because of this, PTHS is often misdiagnosed as Angelman syndrome.
- Children with PTHS can sometimes get frustrated and upset when they cannot communicate what they want or what they are thinking.
Developmental symptoms
- Children and adults with PTHS have moderate to severe learning disability.
- Children with PTHS reach developmental milestones, like rolling over, sitting and walking, later than other children.
- Most children with PTHS will not learn to speak, although some children learn to say a few words and a few children learn to speak quite well. Teaching children to use sign language and pictures is very important to help them communicate.